Doctors adopt aerospace technology for shoulder replacements to improve outcomes for patients
Sign up now: Get ST's newsletters delivered to your inbox

Dr Wong Yoke Rung (left) and Associate Professor Denny Lie (right), shows a 3D-printed model of a shoulder to patient Eric Low (centre), on March 30.
ST PHOTO: AZMI ATHNI
- SGH surgeons use aerospace technology (Finite Element) to simulate shoulder replacement outcomes, predicting implant behaviour and long-term survival.
- Asian patients need smaller implants. SGH uses CT scans and 3D-printed guides for precise, individualised surgery, improving outcomes without raising costs.
- Patient Eric Low experienced painless recovery and improved mobility after shoulder replacement using FE analysis, enabling his active lifestyle.
AI generated
SINGAPORE - Having a total shoulder replacement can change the life of a patient with debilitating shoulder pain and mobility issues.
Now, surgeons and bioengineers at the Singapore General Hospital (SGH) have taken a huge step further by adopting aerospace technology to simulate post-operative outcomes and predict how the implant, bone and soft tissues will interact and how long the implant might last.
Associate Professor Denny Lie, a senior consultant in the Department of Orthopaedic Surgery at SGH, told The Straits Times: “As surgeons, we must consider factors such as the patient’s bone quality, wear patterns and rotator cuff integrity to decide on the best surgical approach, besides selecting the right implant type and size.”
He noted that the bones of the Asian shoulder, especially those of Asian women, are very small.
“Most implants, however, are designed for our Western counterparts,” said Prof Lie, who is also the lead in cell and tissue bioengineering at the hospital.
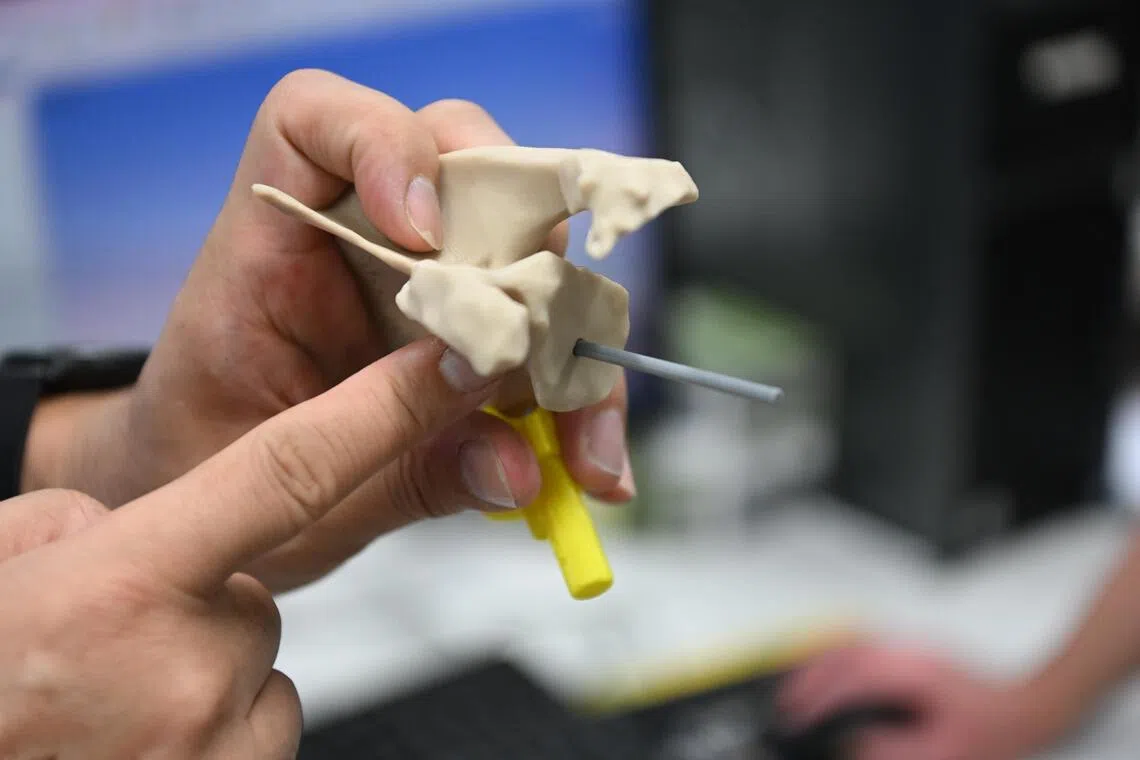
A 3D-printed model of a shoulder printed at the Biomechanics Laboratory in SGH, prior to a shoulder replacement surgery. It has become a standard practice for orthopaedic surgeons but will not push up costs.
ST PHOTO: AZMI ATHNI
“So we used CT scans, virtual surgical planning, and we rehearsed every surgery on the computer. Based on that, we even printed a 3D guide, which is unique for every patient, to practise. I believe it is the way forward – individual precision guide for every patient,” he said.
On average, SGH performs 40 shoulder replacements each year. Prof Lie and his surgical team use between four and five years’ worth of data to lay the virtual surgical groundwork and develop the 3D planning to prepare for every shoulder replacement surgery.
Prof Lie gave the assurance that it will not push up the cost of the procedure. “It just develops the technique and it has become our surgical routine,” he added.
On top of this, they also use a method called finite element (FE), a technology used in aerospace engineering to analyse the aerodynamic effect on the airplane design and ensure its safety and durability.
Dr Wong Yoke Rung, a senior research fellow at the Biomechanics Lab in SGH, said that using the FE method, aerospace engineers build a one-to-one scale air tunnel and have a very big fan on one end and plug sensors on the airplane structure. This is to measure parameters such as forces and vibrations. With this data, they can do virtual testing and adjust designs.
“That set us thinking – why not use it for biomechanical engineering? We can use the same concept to analyse shoulder movement before and after the implant, and simulate the forces and stressors to gather data,” Dr Wong said.
Prof Lie added: “This virtual testing environment allows us to evaluate multiple surgical scenarios before entering the operating theatre, potentially leading to more optimised, patient-specific outcomes.
“By creating detailed digital models that segment the shoulder’s intricate anatomy, the technology can predict how specific surgical decisions – from implant selection and positioning to the patient’s anatomy conditions – affect joint stability and range of motion.”
With FE, the procedure becomes more precise and efficient, and offers improved patient recovery.
One patient who benefited from the FE analysis was former badminton and football coach Eric Low, 67. He told ST of his various injuries over the years that wore down his shoulder.
“In my younger days, I did a lot of outdoor activities; that was how I got all these (joint) injuries. My shoulder injury started in my teens when I was doing the parallel bars during gymnastics. I slipped and my shoulders went ‘boom’,” he said.
He also played softball in school “and whenever I threw the ball, my shoulder would get dislocated”.
“As a young man, I also guided people up Mount Ophir in Malaysia. I almost fell off a few times... The people I guided also slipped, and... I would hold on to the rope to stop the plummeting weight. The jerk did not help my already injured shoulder,” he said.
Possibly as a result of his activities and his job as a badminton and football coach, both of his knees and shoulders required some form of repair.
Since 2016, Mr Low has undergone replacement surgery for his knees and right shoulder. He did the left shoulder replacement in September 2025, and it was done with FE analysis.
“After the operation, I did not have any pain at all, unlike when I went through my knee surgery. The excruciating pain lasted two weeks, and once in a while, morphine needed to be administered.”
Mr Low said that prior to the latest surgery, “I could lift my left arm only to my chest level, and even then, I was already trembling and shaking from the pain. Now I can lift it easily above my head”.
Now that he has recovered, Mr Low is counting down the months till he retires from his administrative job at the Institute of Technical Education in 2027.
“After that, I will continue my active lifestyle and travelling to see the world,” he said.
Prof Lie said this surgery is particularly good for seniors. “Many are still super active. We want them to remain active; that is why we need to optimise their function and ability to continue exercising and leading a full life,” he said.
Higher accuracy, fewer complications
What the finite element method is
Aerospace engineers use the finite element method to break down complex aircraft structures to analyse and accurately predict how a whole aircraft would respond to forces during flight and landing.
In healthcare, Singapore General Hospital (SGH) surgeons and biomechanical engineers use the method to similarly simulate post-operative outcomes in shoulder replacements. It predicts how specific surgical decisions – from implant selection and positioning to patient’s anatomy conditions – affect joint stability and range of motion in the long run.
How the method works
1. A 3D-printed model is created from high-quality images taken via CT scans, magnetic resonance imaging, X-rays, and a patient’s data.
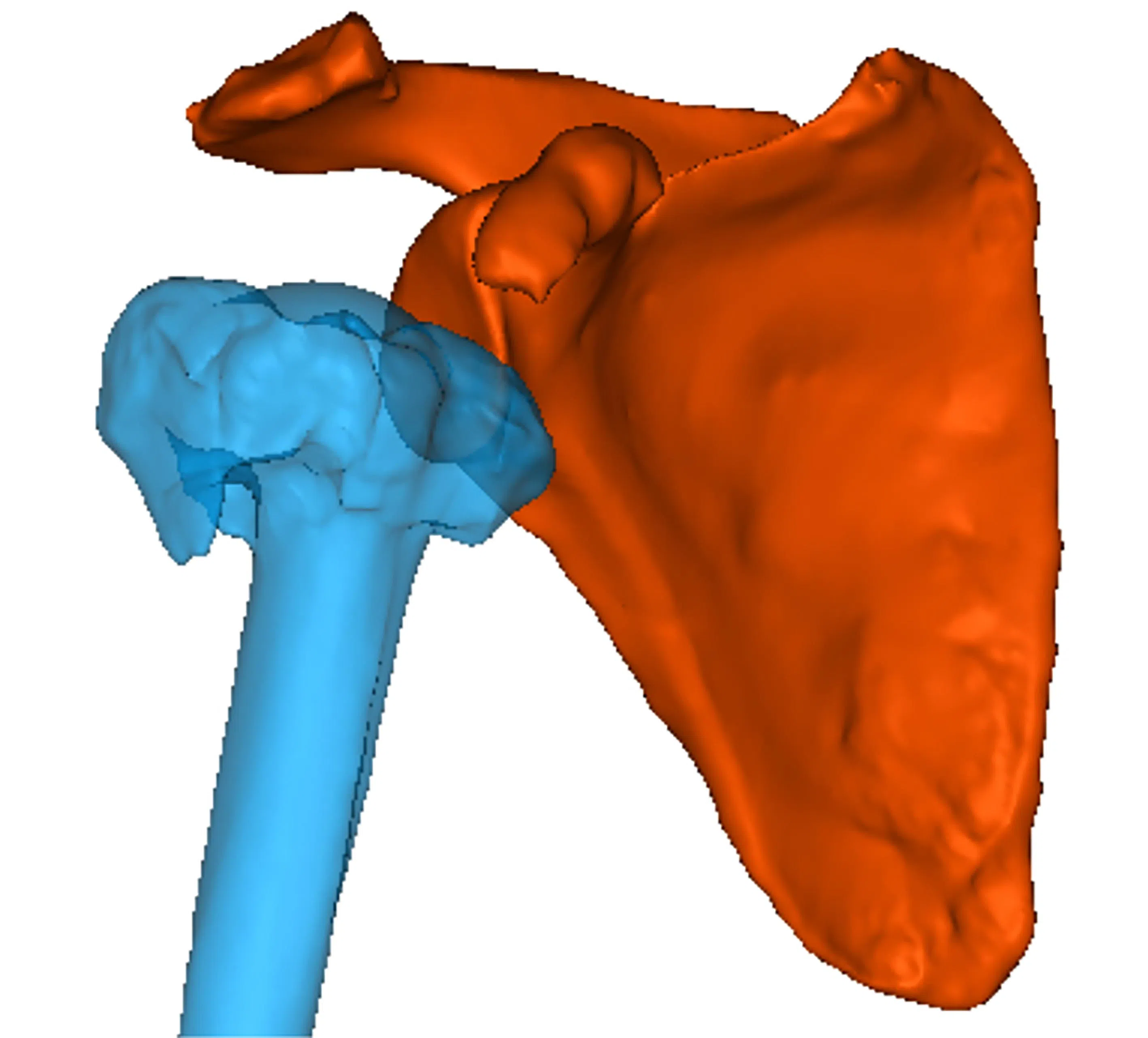

2. A surgeon and a biomechanical engineer create precise digital models. This is to optimise implant positioning and sizing by using virtual surgical planning – a technology-driven, 3D-simulation process to plan and rehearse the procedure.
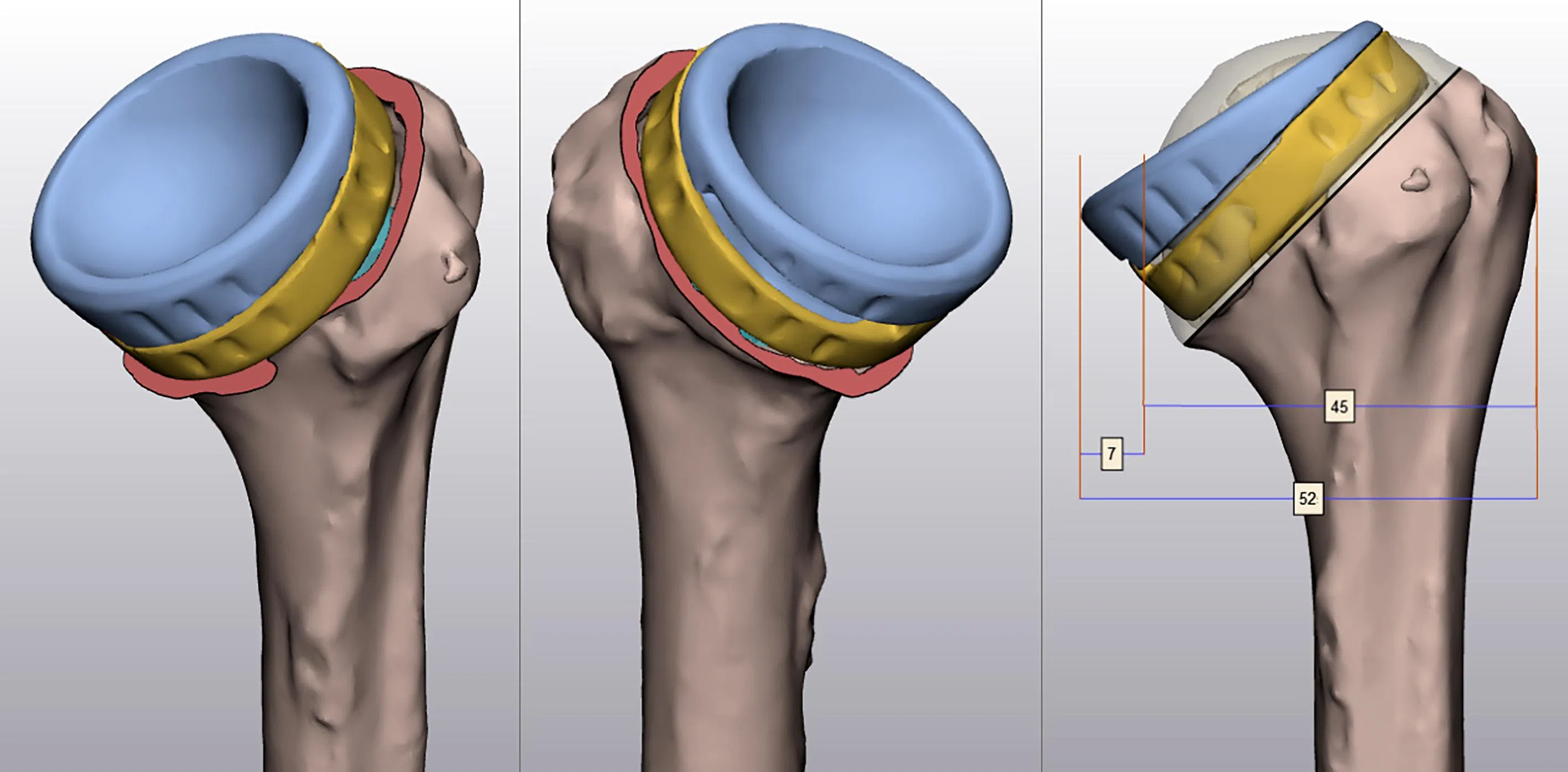
3. The virtual surgical planning of the humerus implant used in shoulder replacements results in higher accuracy, and reduces surgical time and complications.
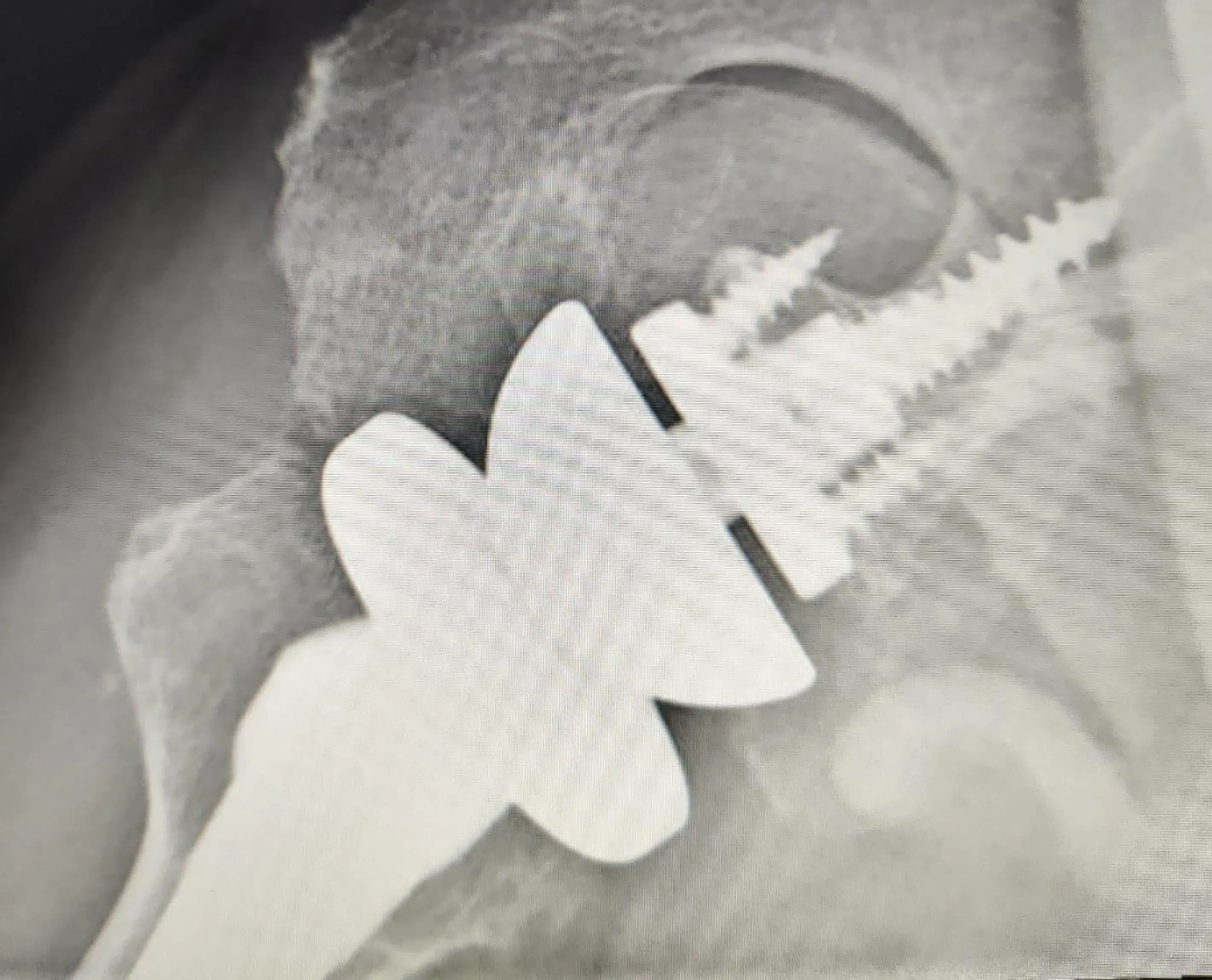
Software tools are used for finite element analysis, and computational modelling is used to simulate biomechanical behaviour under various conditions. The different colours show varying levels of loading on the shoulder.
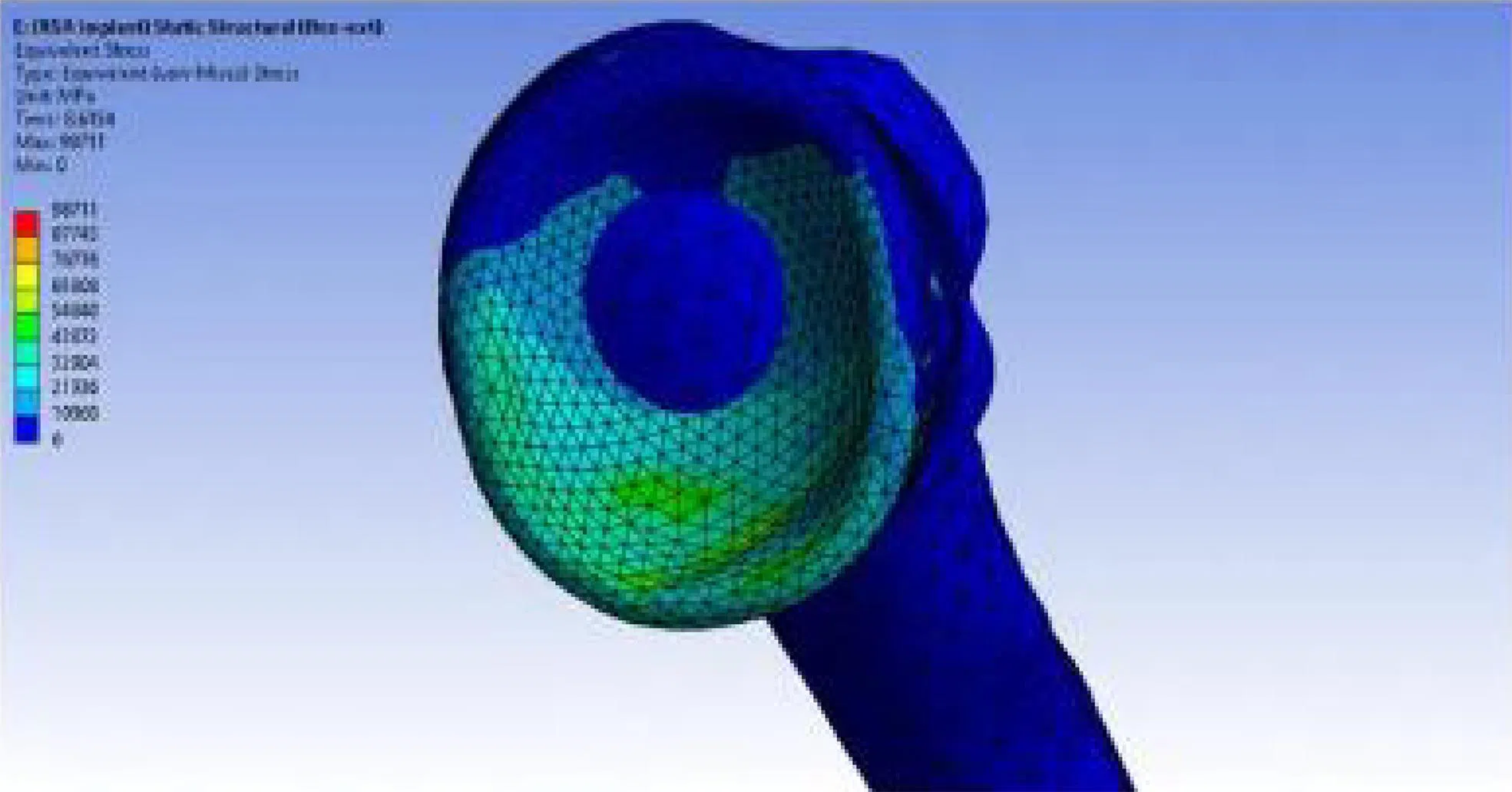
Source: SGH; PHOTOS: SGH, ADOBE STOCK



